L. Iaccarino, S.C. Burnham, G. Dell’Agnello, S.A. Dowsett, S. Epelbaum
Eli Lilly and Company, Indianapolis, IN, USA
Corresponding Author: Leonardo Iaccarino, Avid Radiopharmaceuticals (a wholly owned subsidiary of Eli Lilly and Company, Indianapolis, IN, USA), 3711 Market St., Philadelphia, PA 19104, USA, Ph. +1-215-298-0700, Fax +1-215-754-4950, iaccarino_leonardo@lilly.com
J Prev Alz Dis 2023;3(10):426-442
Published online April 6, 2023, http://dx.doi.org/10.14283/jpad.2023.43
Abstract
Amyloid and tau biomarkers for Alzheimer’s disease are widely recognized diagnostic tools for the identification of Alzheimer’s disease pathology antemortem and are recommended by the most recent clinical and research guidelines. Approved biomarkers include positron emission tomography (PET)- and fluid-based markers derived from cerebrospinal fluid and, more recently, plasma. These biomarkers are still infrequently used in clinical practice, potentially due to challenges in access to and understanding of individual assay information and methodology. We provide an overview of the diagnostic biomarkers for amyloid and tau pathology that are currently available in the US and/or EU for clinical use. Available performance data from both labels/instructions for use and the scientific literature (with focus on autopsy or PET as standard of truth) are summarized to help healthcare providers navigate the biomarker landscape. All available PET amyloid and tau biomarkers demonstrate high accuracy in identifying amyloid and tau Alzheimer’s disease pathology, respectively, at autopsy. Among cerebrospinal fluid biomarkers, all showed accurate prediction of Alzheimer’s disease pathology, either based on autopsy or PET findings; greater accuracy was evident for concentration ratios (Aβ42/40 or P-tau181/Aβ42) versus individual biomarker concentrations. Among plasma biomarkers, Aβ42/40 and P-tau181 demonstrated high agreement with PET findings. Overall, we conclude that commercially available PET, cerebrospinal fluid and plasma assays accurately identify Alzheimer’s disease amyloid and tau pathology. The recent development of fully automated tests for fluid-based biomarkers improves test reliability. The continued development of plasma biomarkers holds promise for the future management of patients with Alzheimer’s disease.
Key words: Alzheimer’s disease, diagnostic biomarker, amyloid, tau.
Introduction
Alzheimer’s disease (AD) is a neurodegenerative disease characterized by progressive cognitive, functional, and behavioral impairment. From a neuropathological standpoint, the 2 hallmarks of AD are the accumulation of extracellular β-amyloid (Aβ) plaques and intracellular neurofibrillary tangles (NFTs). Based on current understanding, the accumulation of Aβ plaques, NFTs and their mutual interactions trigger downstream pathological changes, including neurodegeneration (1). These neuropathological changes may begin decades before they manifest as clinical impairment (2, 3).
Historically, a definitive diagnosis of AD was only feasible through post-mortem examination. This is, in part, a reflection of the shortcoming of clinical diagnosis; it is well recognized that a considerable proportion of individuals with a diagnosis of AD based solely on clinical criteria do not have substantial amyloid and/or tau pathology at autopsy (4). Over the past 2 decades, however, several biomarkers of amyloid and tau pathology have been developed to assist with more accurate ante-mortem diagnosis. Recently (2018), the Amyloid-Tau-Neurodegeneration (ATN) classification was proposed as a research framework that requires abnormal biomarker measures of amyloid (A+) and tau (T+) to diagnose AD with neurodegeneration status (N±) being a non-specific, but useful, indicator of disease stage (5, 6). In this framework, an A+ status is sufficient to place an individual on the AD continuum. It is now the general consensus among leaders in the field that biomarker-confirmed presence of AD pathology is required for a clinical diagnosis of AD (7).
Confirming underlying pathology for AD diagnosis is crucial in light of the continuing focus on the development of disease-modifying therapies (DMTs), including amyloid targeting therapies (ATTs), and the recent positive trial findings. Recent ATT trials, including the donanemab TRAILBLAZER study (8), the aducanumab EMERGE and ENGAGE studies (9), the lecanemab CLARITY AD study (10), and the gantenerumab GRADUATE studies (11) have generally required biomarker confirmation of AD pathology prior to treatment initiation; this helps ensure the study population is appropriate and target engagement is possible. In the clinical trial environment, the use of amyloid and tau biomarkers also allows for disease detection earlier in the continuum (e.g., in the early symptomatic stage) than neurodegeneration markers such as structural magnetic resonance imaging, permitting evaluation of treatments at this stage of disease.
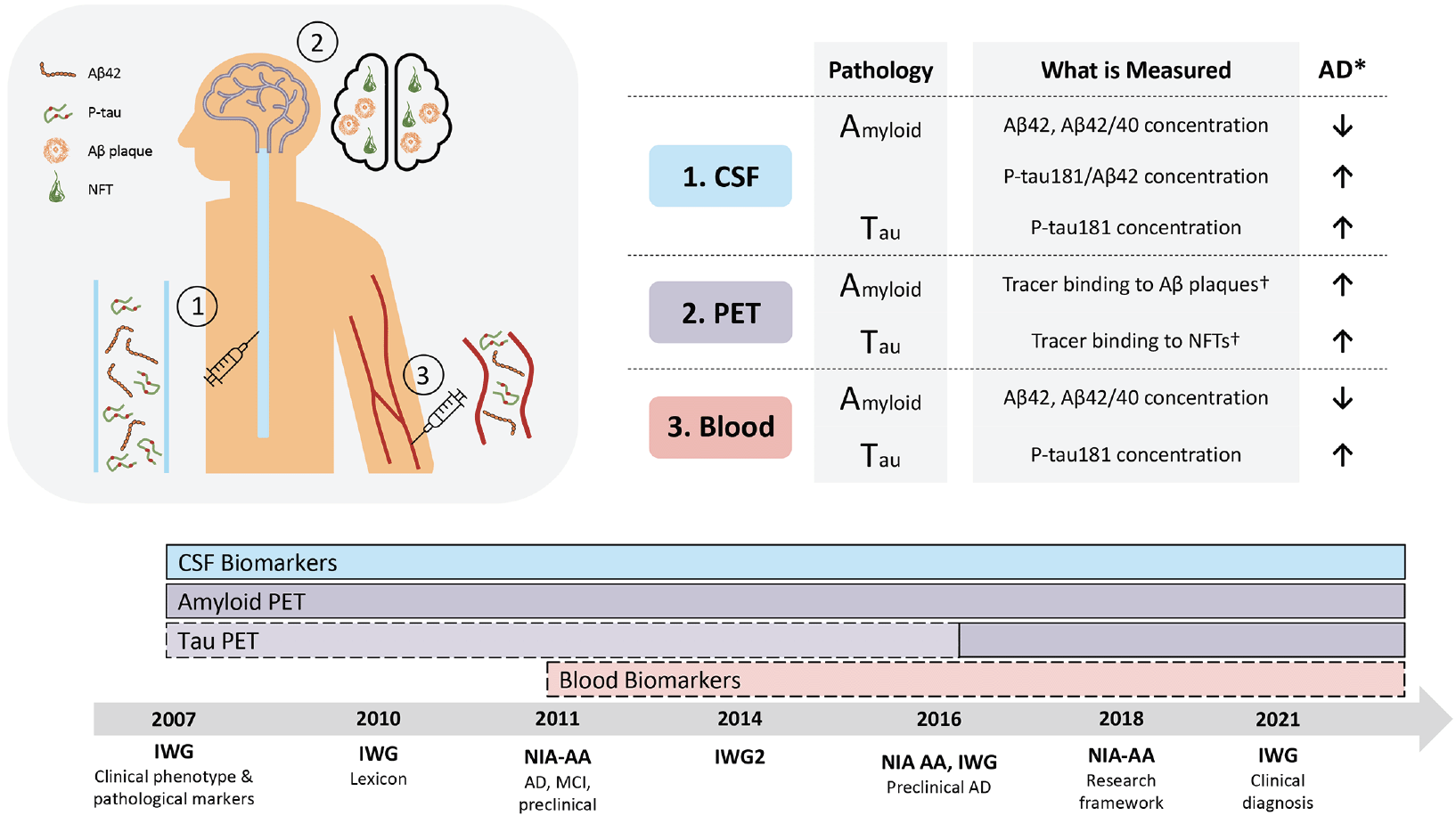
An overview of the development of biomarkers for amyloid and tau pathology, as well as interpretation of biomarker findings, is shown in Figure 1. Approved positron emission tomography (PET) imaging biomarkers employ molecular neuroimaging techniques with amyloid-PET and tau-PET radiotracers, that bind to Aβ plaques and NFTs, respectively. Commercially available fluid-based biomarkers include cerebrospinal fluid (CSF) and plasma Aβ42, Aβ40 and tau hyperphosphorylated at threonine site 181 (P-tau181).
FOOTNOTES: Top left – overview of biomarker detection sites (brain, CSF, blood); Top right – Interpretation of assay findings in amyloid positive (A+) and tau positive (T+) individuals. Individual biomarker assays should be used according to the assay label; *Arrow indicates direction of change in measure in individuals with AD vs healthy individuals †Visual read of PET scan approved for clinical use but PET tracer quantitation now being used in research setting; Bottom – Development timeline includes the diagnostic guidelines established by AD working groups (6, 7, 19-24). Solid line box indicates when biomarker was included in diagnostic guideline; Dashed line box/lighter fill color indicates when biomarker was mentioned in guideline primary manuscript as future consideration; Abbreviations: Aβ, β-amyloid; AD, Alzheimer’s disease; CSF, cerebrospinal fluid; IWG, International Working Group; NIA-AA, National Institute on Aging and Alzheimer’s Association; NFT, neurofibrillary tangles; PET, positron emission tomography
The diagnostic performances of available biomarker tests have been validated using various standards-of-truth (SoTs); these include post-mortem pathology verification and comparing test results from a population with AD to those from healthy individuals or those with other neurogenerative diseases. More recently, given the high predictive value of amyloid- and tau-PET techniques versus the respective pathologies at autopsy (12-15), fluid-based biomarkers are also being validated using PET-based findings as the surrogate SoT.
Despite the growing availability of diagnostic biomarkers in the clinical research environment, their use in clinical practice is limited (16, 17). This is likely the result of multiple factors, including skepticism regarding the role of amyloid, limited availability of disease management options, limited accessibility to or experience with biomarkers, country-specific reimbursement policies, socioeconomic factors and patient hesitancy (17, 18). In addition, accessing and understanding information on the individual tests, including characterization, validation and regulatory status, may be challenging for healthcare providers (HCPs) and, potentially, a barrier to making an informed decision on the use of a specific biomarker test in their practice.
The aim of this review is to provide an overview of the performance of amyloid and tau PET- and fluid-based diagnostic biomarkers authorized by the Food and Drug Administration (FDA) or run as a laboratory developed test (LDT) in the United States (US), or authorized in the European Union (EU). The goal is to provide the relevant information to assist HCPs in navigating biomarker options that could complement clinical and cognitive assessments and support diagnostic decisions.
Methods and terminology
Diagnostic tests were identified through various resources including scientific publications, materials presented at scientific congresses and venues, industry landscape news, and company websites. The criteria for inclusion of a diagnostic test in this review were that it is i) a biomarker of amyloid or tau pathology (hallmarks of AD); and ii) authorized in the US or EU, or run as an LDT in the US, as of August 1, 2022. In vitro diagnostics (IVDs) manufactured and used within health institutions in the EU and research use only (RUO) products in both the EU and US were excluded. Additionally, this review notes whether the diagnostic test has received the FDA’s Breakthrough Device Designation (BDD) (if this information is publicly available). The BDD program is designed to expedite the development and review of medical devices that provide for more effective treatment or diagnosis of a life-threatening or irreversibly debilitating disease or condition.
All available and readily accessible diagnostic performance/agreement parameters reported in the scientific literature and respective official assay documentation (e.g., label or instructions for use) were reviewed. To evaluate the diagnostic accuracy of both PET- and fluid-based biomarkers, we considered autopsy findings as the primary reference standard (or SoT) and report autopsy validation data where available. Where not available (for some fluid biomarkers) PET findings were considered the SoT; this was deemed appropriate in light of the robust ability of amyloid and tau PET to predict pathology at autopsy, as discussed below. The company assay documentation (e.g., instructions for use) was located online or provided to us directly by the company; in the few cases where relevant documentation was not available to us, we refer the reader to the company website(s) to request information.
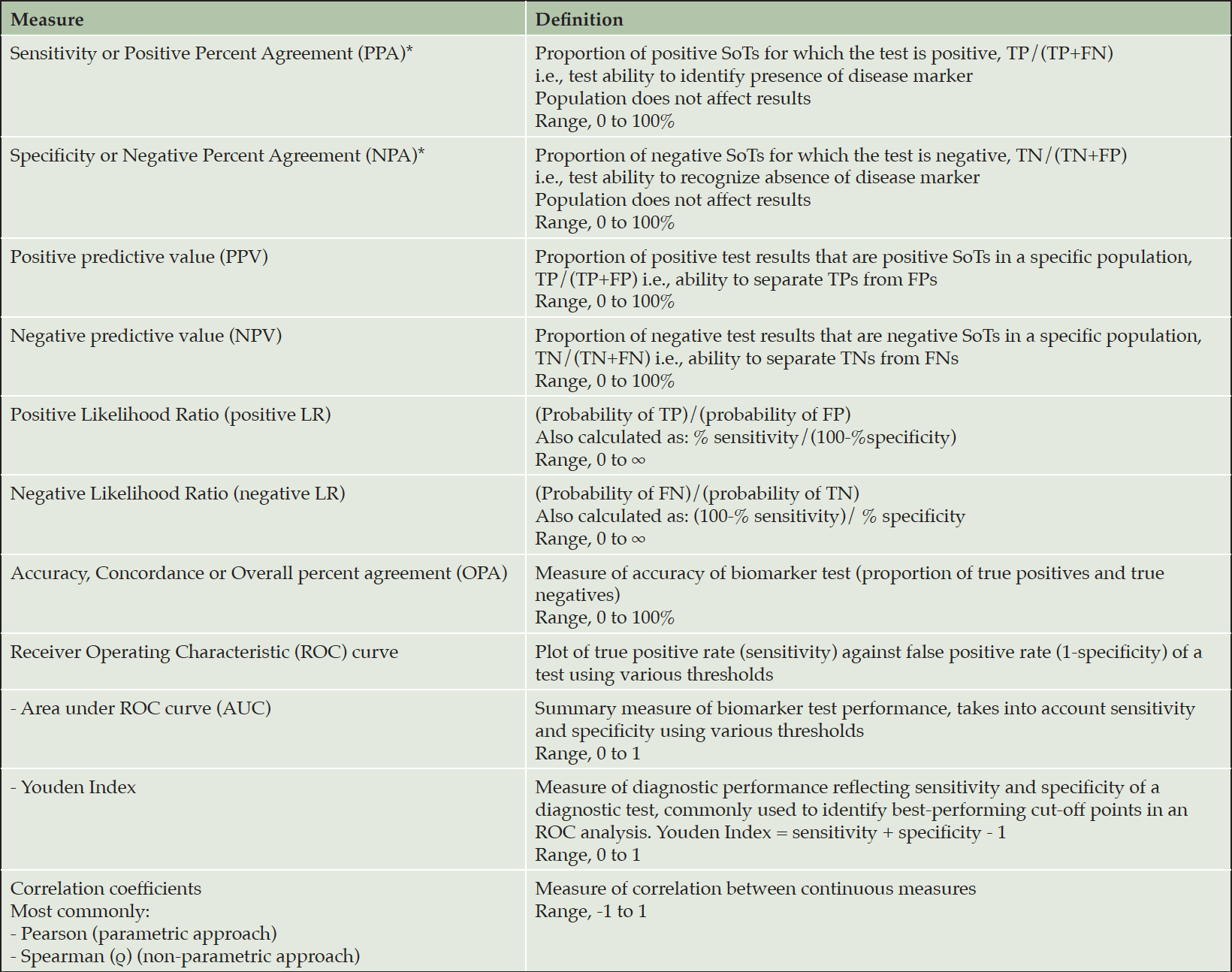
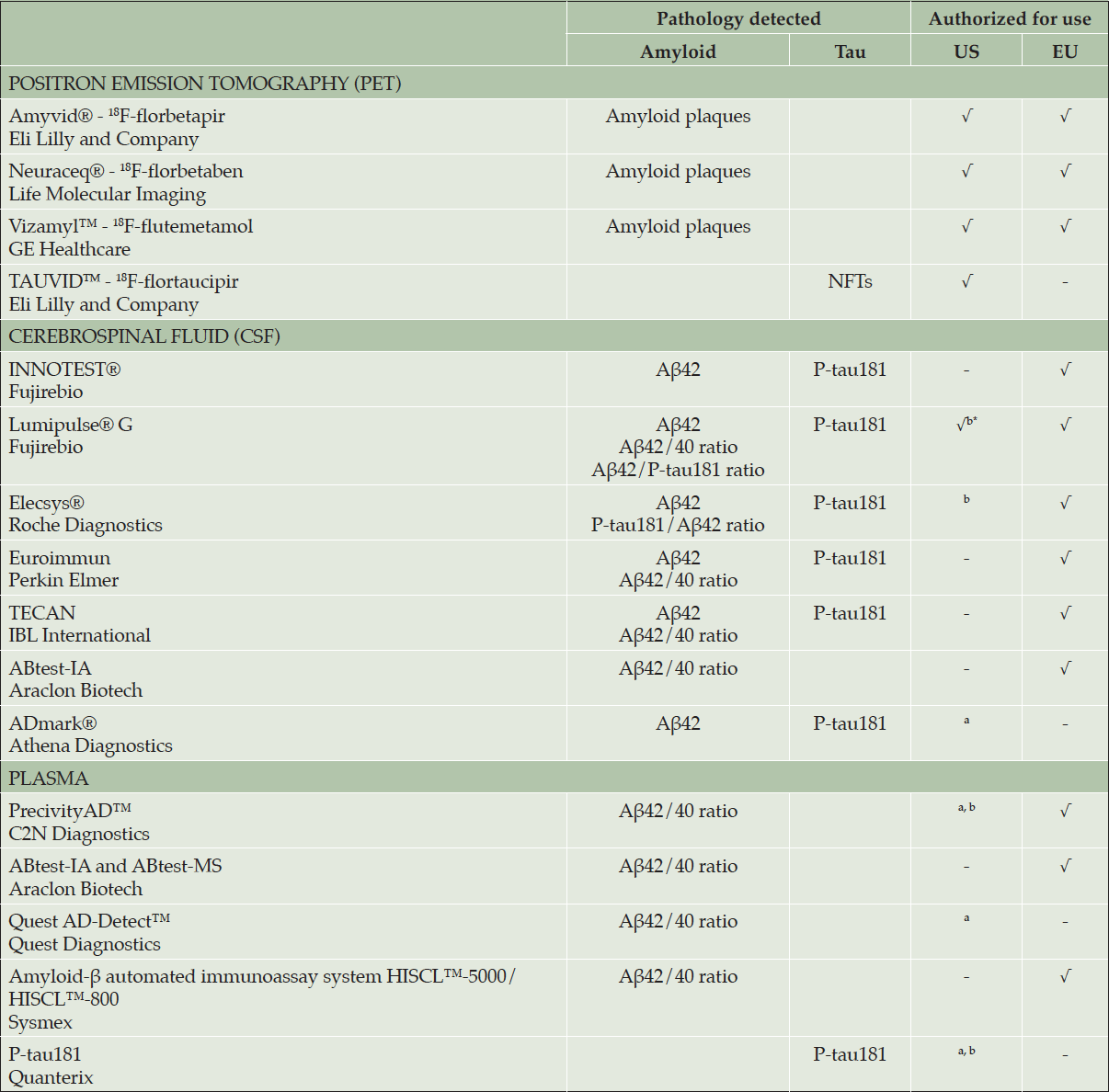
Table 1 provides definitions of the diagnostic performance parameters used in this review. Table 2 provides an overview of the current landscape, while the supplementary table provides a more detailed overview of the findings presented in the text.
FOOTNOTES: *Sensitivity and specificity terminology used where the SoT is the reference standard, i.e., autopsy findings. PPA and NPA terminology used where the SoT is not the reference standard but the best available surrogate, i.e., PET findings. Abbreviations: TP, true positive; TN, true negative; FP, false positive; FN, false negative; SoT, standard of truth
FOOTNOTE: For PET tracers, authorizations equate to FDA or EU Commission approval; In vitro diagnostic (IVD) authorization in EU equates to CE marking; a. Run as a Laboratory Developed Test (LDT); b. Has received FDA’s Breakthrough Device Designation (BDD); *Aβ42/40 ratio only; Abbreviations – AD, Alzheimer’s disease; Aβ, β-amyloid; NFT, neurofibrillary tangle
Positron emission tomography
PET is a molecular imaging technique that uses radiotracers that bind to specific proteins or processes of interest; the location/extent of radiotracer signal is used as a surrogate for the location and number of binding sites, and is presumed to reflect the degree/presence of a particular target (pathological or functional). For AD pathology, PET radiotracers are employed to show the pattern and density of Aβ plaque (amyloid PET) or NFT pathology (tau PET) in the brain (25). For use in clinical practice, approved radiotracers for amyloid and tau PET require visual interpretation of tracer signal; for each radiotracer, there are specific requirements with regards to the PET reading protocol (see labels for respective indications and examples of positive and negative scans).
In the research setting, amyloid and tau PET scans are also analyzed through a quantitative approach. Most commonly, both target regions (in which binding would suggest ongoing disease process) and reference regions (known to be unaffected by the disease process or without specific binding) are identified and the Standardized Uptake Value ratio (SUVr) is calculated as the ratio between target region and reference region bindings. This quantitative analysis is usually performed in specific regions of interest and is useful for estimating disease severity or tracking longitudinal changes.
In the case of amyloid PET, positive binding patterns are remarkably consistent across individuals and tracers, and thus the chosen target and reference regions are generally similar across studies (26). In line with these observations, the Centiloid workgroup has developed a set of harmonized regions of interest, including frontal, temporal, parietal and precuneus, as well as striatum and insular cortices, to be used for amyloid PET quantitation (27).
In the case of tau PET, quantitative approaches are also used to investigate regional (single or composite) SUVrs in the research realm. To detect the presence of elevated tau in the very early stages of AD, the most informative target regions are generally the mesial temporal and inferior lateral temporo-occipital lobe structures. As the disease advances, additional regions (including the medial and lateral parieto-frontal regions) also display significantly elevated tau PET binding. The most common reference regions for tau PET are the cerebellar cortex or composite white matter regions.
PET findings from qualitative (visual reads) and quantitative methodologies are commonly used in the validation of fluid-based biomarkers.
Amyloid Status
18F-Florbetapir
The pivotal study of florbetapir comprised an end-of-life cohort of 59 participants (clinical diagnosis of AD, n=29; other dementia disorder, n=13; mild cognitive impairment [MCI], n=5; cognitively normal [CN], n=12) (12). For 46 participants, there was less than 1 year between the PET scan and death. Visual binary reads (positive/negative) were performed by 5 readers and findings compared with a neuropathological neuritic plaque density score (Consortium to Establish a Registry for Alzheimer’s Disease [CERAD] score). Employing majority read interpretation (image interpretation made by at least 3 of the 5 readers), florbetapir demonstrated a sensitivity of 92% (95% CI 78-98%), a specificity of 100% (95% CI 80-100%), and an overall accuracy of 95% in detecting moderate-to-frequent plaques. These sensitivity/specificity values are also included in the US and EU labels (28, 29). Findings were similar for the subset of participants who died within 1 year of the PET scan or when quantitation instead of qualitative visual reads were used (12). Of note, a visual quantitative rating demonstrated a significant correlation (Spearman ρ, 0.76; p<0.0001) between florbetapir PET findings and Aβ measured by immunohistochemistry at autopsy in participants who died within 2 years of the scan. In this study, a semiautomated quantitative PET scan analysis was also performed in which florbetapir status demonstrated a sensitivity of 97% (95% CI 85%-100%), a specificity of 100% (95% CI 80-100%) and an accuracy of 98% in detecting moderate-to-frequent neuritic plaques (12). Findings from studies of both the pivotal study cohort and cases from the Alzheimer’s Disease Neuroimaging Initiative autopsy cohort have confirmed quantitative relationships between florbetapir PET binding and frontal Aβ42 and demonstrated the ability of florbetapir to successfully predict Thal (amyloid plaque phase) staging (30, 31).
→ Florbetapir is branded as Amyvid® (Eli Lilly and Company, Indianapolis, IN, USA) in the US and EU (28, 29).
18F-Florbetaben
Findings from 74 participants (clinical diagnosis of AD, n=57; dementia with Lewy bodies (DLB), n=3; other dementia disorder, n=6; no dementia, n=8) of the Phase 3 study are reported by Sabri et al (13). For 46 participants there was less than 1 year between the PET scan and death. Visual binary reads were performed by 3 readers and findings compared with CERAD neuritic plaque density score. Employing majority read interpretation, florbetaben demonstrated a sensitivity of 98% (95% CI 94-100%) and a specificity of 89% (95% CI 77-100%) in detecting moderate-to-frequent CERAD scores; the negative predictive value (NPV) was 96% (95% CI 88-100%) and the positive predictive value (PPV), 94% (95% CI 87-100%). Regional majority visual reads across the middle frontal, anterior cingulate and posterior cingulate/precuneus regions showed 82-90% sensitivity and 86-95% specificity in detecting moderate neuritic/cored or diffuse plaques, with a significant correlation between quantitated florbetaben PET binding and histopathological scores. Using a quantitative approach, composite SUVr predicted CERAD neuropathology score with an area under the curve (AUC) of 0.91, 89% sensitivity and 92% specificity.
In the US label (32), findings from 82 participants of the Phase 3 cohort are reported; the median sensitivity and specificity of florbetaben PET were 98% and 80%, respectively. Findings from 31 participants of the Phase 3 cohort are included in the EU label (33); based on a majority read, the sensitivity of florbetaben PET was 100% and the specificity, 86%.
In 2 additional studies that included participants from the Phase 3 cohort, findings from several florbetaben PET quantitation approaches (with various target and reference regions as well as image processing pipelines) were compared with Aβ histopathology findings (both neuritic plaque and diffuse plaque scores) at autopsy. The AUC, sensitivity and specificity ranges were 0.84-0.97, 87-96% and 60-96%, respectively (34, 35).
→ Florbetaben is branded as Neuraceq® (Life Molecular Imaging, Berlin, Germany) in the US and EU (32, 33)
18F-Flutemetamol
A pivotal flutemetamol Phase 3 study included an end-of-life cohort of 68 participants, (clinical diagnosis of AD, n=30; other dementias, n=17; no history of cognitive impairment, n=21) (14). Flutemetamol PET was performed on average 3.5 (range 0-13) months before death. Visual binary reads were performed by 5 readers and findings compared with modified CERAD neuritic plaque density scores at autopsy. Majority reads of flutemetamol scans demonstrated an AUC of 0.90 (95% CI 0.82-0.97), a sensitivity of 86% (95% CI 72-95%) and a specificity of 92% (95% CI 74-99%); the sensitivity/specificity values were also included in the EU label (36). In the US label (37), median performances across readers were provided (88% sensitivity, 88% specificity).
In the Phase 3 study, of those participants with an advanced amyloid plaque score at autopsy (Thal phase 4-5), 89% of flutemetamol PET scans were rated positive, while of those with none/low score (Thal Phase 0-2), 100% of scans were rated negative. For those at Thal Phase 3, 33% were rated positive (38). Additional studies of this Phase 3 cohort plus additional participants (total N=106) confirmed the flutemetamol PET majority read performance in predicting Aβ histopathology, using a modified CERAD score and the Thal score as well as other categorical neuropathology SoTs (39, 40). Flutemetamol PET demonstrated an AUC of 0.89-0.96, a sensitivity of 79-100% and a specificity of 65-100%, depending on the adopted SoT. In a subset of 28 participants from the original Phase 3 cohort, the overall agreement between flutemetamol PET visual read and neuritic plaque density at autopsy was 89% (41).
→ Flutemetamol is branded as Vizamyl™ (GE Healthcare, Arlington Heights, IL, USA) in the US and EU (36, 37).
Tau Status
Currently, only one tau PET radiotracer (flortaucipir) is approved for clinical use in the US; none are approved in the EU.
18F-Flortaucipir
The pivotal study of flortaucipir comprised an end-of-life primary cohort of 64 participants (dementia, n=49; MCI, n=1; CN, n=14) (15). PET scans were performed, on average, 2.6 months before death. Visual binary reads were performed by 5 readers and findings compared with Braak NFT pathological staging at autopsy; level B3 (Braak stages V or VI; NFTs throughout neocortex) was considered positive. Majority reads of flortaucipir scans demonstrated a sensitivity of 92% (95% CI 80-97%) and a specificity of 80% (95%CI 61-91%) in predicting an NFT B3 score. The US label (42) includes sensitivity and specificity of individual readers only; with a calculated median sensitivity of 92% and specificity of 76%. Considering a high Alzheimer’s Disease Neuropathologic Change (ADNC) score (incorporates Thal amyloid plaque phase [Phase 4-5], CERAD neuritic plaque density [at least moderate-to-frequent] and Braak NFT staging [at least Braak V/VI]) as the neuropathology SoT, flortaucipir PET majority reads demonstrated a sensitivity of 95% (95% CI 83-99%) and specificity of 81% (95% CI 62%-92%). The inclusion of an additional 18 participants (dementia, n=11; MCI, n=3; CN, n=4) yielded similar findings with both Braak pathological staging and ADNC score comparators.
A study of 143 participants evaluated the ability of flortaucipir PET to discriminate between autopsy-confirmed frontotemporal lobar degeneration (FTLD), low/intermediate and high ADNC. Greatest differentiation between FTLD and high ADNC was observed using the midbrain/inferior temporal binding ratio (AUC 0.99 ([95% CI 0.94-1.00]; sensitivity 94%; specificity 95%) while the greatest differentiation between low/intermediate and high ADNC was observed using the entorhinal cortex binding ratio (AUC 0.94 [95% CI 0.85-0.97]; sensitivity 88%; specificity 88%). The midbrain/inferior temporal binding ratio was the top performer, although with lower accuracy, when comparing FTLD to low/intermediate ADNC (AUC 0.80 [95% CI 0.68-0.88], sensitivity 71% and specificity 70%)(43). Overall, these findings support the view that flortaucipir PET accurately identifies advanced Braak B3 level (Braak V/VI stages). Smaller studies have reported that elevation of flortaucipir PET binding is more consistently observed in patients with advanced Braak stages (44, 45). In addition, regional flortaucipir PET binding shows a significant correlation with co-localized quantitative tau neuropathology findings, such as those from P-tau immunohistochemistry, at autopsy (45-47).
→ Flortaucipir is branded as TAUVIDTM (Eli Lilly and Company, Indianapolis, IN, USA) in the US (42).
CSF Biomarkers
CSF analysis is a well-established and clinically useful approach to investigate AD pathophysiology (48-50). Compared with PET, it is more accessible and cost-effective, less resource intensive and does not require exposure to radioactivity. While generally a safe procedure, CSF analysis requires a lumbar puncture (spinal tap). It may be affected by pre-analytical factors and, unlike PET, does not provide direct information on protein aggregation (18, 50).
Over the last 2 decades, several CSF measures have been validated and approved by the FDA and European Medicines Agency (EMA) for the assessment of amyloid and tau pathology in AD antemortem. Historically, CSF measures of interest were Aβ42, P-tau181 (tau hyperphosphorylated at threonine 181) and T-tau (total tau); more recently, Aβ42/40 and the P-tau181/Aβ42 ratios have been shown to accurately identify AD using different SoTs. Although we consider amyloid and tau pathology biomarker findings as indicators of amyloid and tau status, respectively, in some instances tau biomarker assays (e.g., Lumipulse® G P-tau181) have been validated with SoTs indicative of amyloid pathology (amyloid PET). This is discussed further in the Predicting amyloid/tau status through tau/ amyloid biomarker findings section.
The concentrations of CSF biomarkers can be measured with various technologies, including but not limited to enzyme-linked immunosorbent assay (ELISA), immunoassay with electrochemiluminescence detection (ECL, sometimes referred to as ECLIA), chemiluminescence enzyme immunoassay (CLEIA), and single molecule array (Simoa); this topic was recently reviewed by Zetterberg and Blennow (51).
Amyloid Status
CSF Aβ42 and Aβ42/40 ratio
Aβ42 is the main component of the amyloid plaques characteristic of AD, and the current hypothesis suggests that lower CSF Aβ42 concentrations reflect its aggregation and sequestering in brain amyloid plaques (51). The most well-established CSF amyloid biomarkers are the Aβ42 isoform concentrations and the ratio between the Aβ42 and Aβ40 isoforms (Aβ42/40). The ratio approach is based on the belief that the Aβ40 concentration can serve as a reference and that using the basal total Aβ (which varies between individuals) to normalize Aβ42 concentrations can improve overall diagnostic accuracy (52, 53). Both Aβ42 level and Aβ42/40 ratio, when decreased compared to normative values, indicate ongoing amyloid pathology. The accuracy of CSF Aβ biomarkers in reflecting ongoing AD amyloid plaque pathology has been generally validated using autopsy confirmation as gold standard. More recently, in light of its robust performance in predicting amyloid pathology at autopsy, amyloid PET has also been used as the SoT for CSF Aβ42 and Aβ42/40 validation.
INNOTEST® (Fujirebio, Tokyo, Japan) – ELISA
The ability of INNOTEST (measuring CSF Aβ42 concentration) to predict the presence of neuritic plaque at autopsy was evaluated in a study of 123 participants (clinical diagnosis of AD, n=79; other dementia, n=29; other neurological disease, n=15), with a median interval between lumbar puncture and death of 13-34 months depending on disease subgroup (54). INNOTEST CSF Aβ42 showed an AUC of 0.87 (95% CI 0.78-0.95), a sensitivity of 80% and a specificity of 82%; this translated to a positive likelihood ratio (LR) of 4.5 (95% CI 2.0-10) and a negative LR of 0.24 (95% CI 0.16-0.38).
Of note, this study and others (54-56), have demonstrated a significant inverse correlation between CSF Aβ42 concentrations (lumbar or ventricular) and Aβ histopathology (Aβ load or plaques density) at autopsy or frontal biopsy. Such correlation is likely to be weaker in more advanced disease stages where CSF Aβ42 may reach equilibrium and is thus not optimally reflective of brain amyloid load in later disease stages (57).
One smaller study (N=21) showed INNOTEST CSF Aβ42 to have a 91% sensitivity and 60% specificity in differentiating between AD and non-AD primary neuropathological diagnosis at autopsy (58), while another small study (N=17) showed that a CSF AD profile (combining Aβ42 and P-tau181 findings), compared with an AD vs non-AD neuropathological diagnosis, had an overall percent agreement (OPA) of 85% (15/17 cases) (59). INNOTEST CSF Aβ42 demonstrated a 92% sensitivity and 75% specificity in differentiating between Thal phases 0-2 and 3-5, and a 90% sensitivity and 55% specificity in differentiating between CERAD none-to-sparse and moderate-to-frequent stages.
The EU instructions for use (60) includes INNOTEST CSF Aβ42 findings based on a clinical SoT (individuals with AD [n=150] versus healthy controls [n=100] and individuals with other neurological disorders [n=84]); INNOTEST CSF Aβ42 demonstrated an 85% positive percentage agreement (PPA) and a 55% negative percentage agreement (NPA).
→ INNOTEST® CSF Aβ40 and Aβ42 are CE marked in EU (60).
Lumipulse® G (Fujirebio, Tokyo, Japan) – CLEIA
To our knowledge, there are currently no published data on the performances of Lumipulse G CSF Aβ42 and CSF Aβ42/40 in predicting amyloid pathology at autopsy. Several studies have, however, investigated the accuracy of Lumipulse G CSF amyloid biomarkers using amyloid PET positivity (evaluated through visual read or quantitation analysis) as the SoT. Across larger studies (>50 participants), Lumipulse G (measuring CSF Aβ42 concentration) showed AUCs of 0.76-0.92, PPAs of 80-99%, NPAs of 50-88% and OPAs of 72-90% compared to amyloid PET (visual read or quantitation) (61-63). Lumipulse G CSF Aβ42/40 ratio generally demonstrated improved performance, with AUCs of 0.86-0.94, PPAs of 77-99%, NPAs of 77-98% and OPAs of 84-92% (61, 63-65). Similar performances were observed in a smaller study using both visual read and quantitation to define amyloid PET positivity (66).
In the EU instructions for use (60), the performances of Lumipulse G CSF Aβ42 and Lumipulse® G CSF Aβ42/40 ratio were tested in a cohort of 94 participants (the majority with AD or DLB). In the prediction of amyloid PET positivity (florbetapir, visual read), Lumipulse G CSF Aβ42 showed an AUC of 0.76 (95% CI 0.65-0.86), 95% PPA and 51% NPA using a receiver operating characteristic (ROC)-defined threshold based on Youden index. Lumipulse® G CSF Aβ42/40 ratio demonstrated an overall improved performance with an AUC of 0.87 (95% CI 0.77-0.96), 88% PPA and 80% NPA. In the EU instructions for use for Lumipulse G P-tau181 (60), Lumipulse G Aβ42/P-tau181 showed an AUC of 0.88 (95% CI 0.79-0.97), with 93% PPA and 80% NPA.
In the EU instructions for use (60), finding from a study in which Lumipulse G CSF Aβ42 and Lumipulse G CSF Aβ42/40 ratio were also tested using a clinical SoT were included. In differentiating AD (n=60) versus non-AD neurological disorders (n=43), Lumipulse G CSF Aβ42 had an AUC of 0.83 (95% CI 0.75-0.92), 78% PPA and 81% NPA; Lumipulse G CSF Aβ42/40 ratio had an AUC of 0.98 (95% CI 0.95-1.00), 98% PPA and 91% NPA. In the EU instructions for use for Lumipulse G P-tau181 (60), Lumipulse G Aβ42/P-tau181 showed 95% PPA and 98% NPA.
The US IVD label (60, 67) includes findings from a study of 292 participants (AD, n=104; late MCI, n=59; early MCI, n=111; subjective cognitive decline, n=18). Lumipulse G (Aβ42/40 ratio) demonstrated 92% PPA and 93% NPA versus amyloid PET (visual read), excluding “likely positive” cases; including these likely positive cases, the PPA was 92% and the NPA was 84%.
→ Lumipulse® G CSF Aβ42/40 ratio has BDD and is IVD approved in the US (60, 67, 68).
→ Lumipulse® G CSF Aβ40 and Aβ42 are CE marked in EU (60).
Elecsys® (Roche Diagnostics, Rotkreuz, Switzerland) – ECLIA
A study of 101 participants with heterogenous neuropathologic diagnoses (including AD and FTLD) evaluated the ability of Elecsys immunoassays to discriminate none-low from intermediate-high ADNC at autopsy; CSF Aβ42 demonstrated an AUC of 0.89 (95% CI 0.81-0.96) for (69). Similar performances were observed in a smaller scale study (N=45), where Elecsys CSF Aβ42 showed AUCs of 0.91 (95% CI 0.81-1.00) in predicting an intermediate-to-high Thal score, 0.83 (95% CI 0.68-0.99) in predicting an intermediate-to-high CERAD neuritic plaque score and 0.92 (95% CI 0.83-1.00) in predicting an intermediate-to-high CERAD diffuse plaque score (70). In the EU instructions for use, (71) findings from 277 participants (subjective cognitive decline, n= 120; MCI, n=153, no assignment, n=4) from the BioFINDER cohort were reported; Elecsys CSF Aβ42 demonstrated an AUC of 0.87 (95% CI 0.82-0.91), an OPA of 80%, a PPA of 91% (95% CI 84-96%), and an NPA of 73% (95% CI 65-79%) versus amyloid PET.
Of note, the P-tau181/Aβ42 ratio findings were also included in the EU label (71) where an AUC of 0.94 (95% CI 0.92-0.97), a PPA of 91% (95% CI 84-96),and an NPA of 89% (95% CI 84-94%) versus amyloid PET were reported.(69) In the previously-cited study of 45 participants, Elecsys P-tau181/Aβ42 ratio showed AUCs of 0.96 (95% CI 0.90-1.00), 0.98 (95% CI 0.94-1.00) and 0.97 (95% CI 0.92-1.00) in predicting an intermediate-to-high Thal score, intermediate-to-high CERAD neuritic plaque score and intermediate-to-high CERAD diffuse plaque score, respectively (70).
→ Elecsys® Aβ42 is CE marked in EU (71) and has FDA BDD in the US (72).
→ Elecsys® P-tau181 is CE marked in EU (73) and has FDA BDD in the US (72).
Euroimmun (Perkin Elmer, Waltham, MA, USA) – ELISA
To our knowledge, there are no published findings on the relationships between Euroimmun CSF Aβ42 or Aβ42/40 ratio and autopsy findings. Rather, studies have employed amyloid PET as the SoT. Large studies of clinically heterogenous cohorts have demonstrated that Euroimmun CSF Aβ42 predicts amyloid PET positivity with a high degree of accuracy, with AUCs of 0.81-0.89, PPAs of 78-83% and NPAs of 69-83%. Euroimmun CSF Aβ42/40 ratio generally showed improved performance, with AUCs of 0.87-0.96, PPAs of 83-100% and NPAs of 72-94% (74-77). Of note, test performance was similar across tracers (flutemetamol and florbetapir), and methods to establish positivity (visual read and quantitation).
A study of 101 participants provides additional performance data for Euroimmun CSF Aβ42 , with a reported OPA of 82% versus amyloid PET, and a significant correlation between assay findings and flutemetamol neocortical binding (Spearman ρ=-0.58, p< 0.001) (78).
The EU instructions for use (79) includes findings based on a clinical SoT (differentiating AD [n=67] from vascular dementia [n=44] and healthy controls [n=43]). Excluding intermediate positive cases, Euroimmun CSF Aβ42 showed 89% PPA, 75% NPA and 81% OPA; including intermediate positive cases, these values were 91%, 66% and 77%, respectively. Euroimmun CSF Aβ42/40 ratio showed overall improved performances with 94% PPA, 76% NPA and 84% OPA.
→ Euroimmun Aβ42 and Aβ40 ELISAs are CE marked in EU (79).
TECAN (IBL International, Hamburg, Germany) – ELISA
A study of 200 participants (CN and cognitively-impaired) assessed the concordance between CSF Aβ42 and amyloid PET (80). Compared with 11C-PiB PET status (positive/negative), TECAN CSF Aβ42 showed an AUC of 0.81 (95% CI 0.75-0.87), a PPA of 82% (95% CI 68-91%), an NPA of 73% (95% CI 65-80%), and an overall concordance of 75%. TECAN CSF Aβ42/40 ratio showed an AUC of 0.94 (95% CI 0.89-0.97), a PPA of 96% (95% CI 86-100%), an NPA of 88% (95% CI 82-93%), and an overall concordance of 89%. The EU instructions for use (81, 82) include performance data based on a sample of 203 individuals (early probable/possible AD or MCI, n=115; controls, n=88); TECAN CSF Aβ42 demonstrated a PPA of 77% and an NPA of 83% in identifying individuals with AD vs controls while for TECAN CSF Aβ42/40 ratio these values were 92% and 94%, respectively.
→ TECAN Aβ40 and Aβ42 are CE marked in EU (83).
ABtest-IA (Araclon Biotech [a subsidiary of Grifols], Zaragoza, Spain]) – ELISA
To our knowledge, there are no published studies on the performance of CSF ABtest-IA using either autopsy-based or amyloid PET based SoTs.
→ ABtest-IA is CE marked in EU (84, 85).
ADMark® (Athena Diagnostics, Marlborough, MA, USA) – ELISA
In a study of 154 participants with presumed normal pressure hydrocephalus and who had a frontal lobe biopsy at the time of shunt placement, the ability of ADMark® CSF Aβ42 to predict neuropathological manifestations of AD was evaluated (86). Using study-specific thresholds, ADMark® CSF Aβ42 showed an AUC of 0.78, with a sensitivity of 93% and a specificity of 54%. Combining CSF Aβ42 and total tau findings into a Aβ42/total tau index (ATI) resulted in an AUC of 0.69, with a sensitivity of 72% and a specificity of 70%.
→ ADMark® is available as LDT for clinical use in the US (87).
Tau Status
CSF P-tau181
The main constituent of the intracellular NFTs, a specific pathological hallmark of AD, is hyper-phosphorylated tau (P-tau). Based on evidence to date, it is generally thought that increased phosphorylation and secretion of tau in AD are related to neuronal exposure to Aβ and are associated with NFT formation (6, 48, 51, 53, 88).
Concentrations of P-tau are of particular relevance to AD diagnosis. In particular, the CSF concentration of P-tau181 is a well-established biomarker for AD (51). Validation of assays measuring CSF P-tau181 has used autopsy-based NFT density or staging (e.g., Braak stages) and, more recently tau PET as the SoT. Of note, CSF P-tau181 concentrations and tau PET findings are likely a reflection of different aspects of tau pathology in AD, with CSF P-tau181 likely indicative of the early response to Aβ and preceding detectable elevation through tau PET (88).
INNOTEST® (Fujirebio, Tokyo, Japan) – ELISA
The performance of P-tau181 concentration, measured using INNOTEST, in predicting the presence of NFTs (Braak stage ≥ I/II) at autopsy was assessed in a study of 123 participants (see INNOTEST Aβ42 and Aβ42/40 ratio section for cohort details). INNOTEST CSF P-tau181 demonstrated an AUC of 0.82 (95% CI 0.68-0.95), a sensitivity of 69% and a specificity of 85%, corresponding to a positive LR of 4.5 (95% CI 1.3-16) and a negative LR of 0.37 (95% CI 0.25-0.53) (54). In the EU instructions for use (60), INNOTEST CSF P-tau181 was reported to have 80% PPA and 87% NPA in identifying individuals with AD versus controls. Using another clinical SoT (AD versus DLB) INNOTEST CSF P-tau181 showed 80% PPA and 79% NPA.
A smaller scale study (N=21) demonstrated a specificity of 100% but a lower sensitivity (73%) for INNOTEST CSF P-tau181 in differentiating between AD and a non-AD primary neuropathological diagnosis at autopsy (58). Additional performance data are provided in a study of 114 participants that showed a significant correlation between INNOTEST CSF P-tau181 and Braak stage (Montine score B (89)), with Spearman ρ of 0.36-0.42, depending on time between lumbar puncture and death (≤4, ≤5 or ≤10 years) (57).
→ INNOTEST® P-tau181 is CE marked in EU (60).
Lumipulse® G (Fujirebio, Tokyo, Japan) – CLEIA
To our knowledge, there are currently no data on the performance of Lumipulse G CSF P-tau181 using either autopsy-based or tau PET based SoTs.
In the EU instructions for use (60), Lumipulse G CSF P-tau181 showed an AUC of 0.84 (95% CI 0.75-0.93) in predicting amyloid PET positivity (18F-florbetapir, visual read). Using a clinical SoT (differentiating AD [n=60] from non-AD neurological disorders [n=43]) Lumipulse G CSF P-tau181 showed an AUC of 1.00 (95% CI 0.99-1.00), 97% PPA and 100% NPA using an ROC-based, Youden-based threshold.
→ Lumipulse® G P-tau181 CLEIA is CE marked in EU (60).
Elecsys® (Roche Diagnostics, Rotkreuz, Swizerland) – ECLIA
In the study of 101 participants with heterogenous neuropathologic diagnoses (see Elecsys Aβ42 and Aβ42/40 ratio section), Elecsys CSF P-tau181 had an AUC of 0.75 (95% CI 0.63-0.87) in differentiating between a none-low ADNC and intermediate-high ADNC (69). In a study of 45 participants, Elecsys CSF P-tau181 demonstrated an AUC of 0.88 (95% CI 0.77-0.99) in identifying intermediate-to-high Braak stage at autopsy (70).
In the EU instructions for use (73), findings from 277 participants from the BioFINDER cohort were reported; Elecsys CSF P-tau181 demonstrated a PPA of 91% (95% CI 84-96%) an NPA of 89% (95% CI 84-94%) and an AUC of 0.94 (95% CI 0.92-0.97) versus amyloid PET.
→ Elecsys® P-tau181 is CE marked in EU (73) and has FDA BDD in the US (72).
Euroimmun (Perkin Elmer, Waltham, MA, USA) – ELISA
To our knowledge, there are no published studies on the performance of Euroimmun CSF P-tau181 using autopsy-based evidence. A study (N=101) did, however, evaluate the performance of Euroimmun CSF P-tau181 versus PET (78). Compared to flortaucipir-PET positivity at quantitation, either estimating binding in the inferior temporal cortex or in more advanced Braak V/VI-like regions, CSF P-tau181 showed concordances of 77% and 65% and Cohen Κ of 0.59 and 0.58, respectively. Correlations (Spearman ρ) were 0.71 and 0.59, respectively.
In a company-published AD document (79), Euroimmun CSF P-tau181 showed an AUC of 0.94, a PPA of 93% and an NPA of 84% in differentiating between individuals with AD (n=61) and healthy controls (n=49).
→ Euroimmun P-tau181 is CE marked in EU (79).
TECAN (IBL International, Hamburg, Germany) – ELISA
To our knowledge, there are no published studies on the performance of TECAN CSF P-tau181 using either autopsy-based or tau-PET based SoTs. The EU instructions for use (82) reports findings from a study of 101 participants (AD/MCI, n=37; control, n=64); TECAN P-tau181 demonstrated an 87% sensitivity and a 92% specificity in differentiating between individuals with AD/MCI and controls.
→ IBL International TECAN P-tau181 is CE marked in EU (82).
ADMark® (Athena Diagnostics, Marlborough, MA, USA) – ELISA
In the previously described study of 154 participants (86), using study-specific thresholds ADMark® CSF P-tau181 showed an AUC of 0.85, with both a sensitivity and specificity of 80%.
→ ADMark® is available as LDT for clinical use in the US (87).
Plasma biomarkers
Recent years have witnessed a rapid development of plasma biomarkers for amyloid and tau pathology, with several assays now authorized in the US or EU or run as LDTs in the US. These biomarkers offer advantages over CSF biomarkers and PET; they are less invasive and have the potential to be more cost-effective. As a result, there is potential for more widespread use and accessibility. Like CSF biomarkers, however, plasma biomarkers do not provide information on location of amyloid or tau pathology and may be affected by pre-analytical factors (related to blood draw/storage). Similarly to CSF biomarkers, various technology platforms are currently being used or tested for plasma biomarkers (90). These platforms include liquid chromatography with tandem mass spectrometry (LC-MS/MS), ELISA and Simoa.
Amyloid Status
Plasma Aβ42/40
PrecivityAD™ (C2N Diagnostics, St Louis, MO, USA) – LC-MS/MS
PrecivityAD incorporates quantification of plasma Aβ42/40 and detection of apolipoprotein E (ApoE)-specific peptide using LC-MS/MS. Plasma Aβ42/40 ratio, ApoE proteotype and patient age are used to determine an amyloid probability score (APS), a measure of the probability that the individual has a positive amyloid PET scan. Initial performance evaluations showed that PrecivityAD Aβ42/40 ratio, in conjunction with ApoE, age and cohort effects, demonstrated an AUC of 0.90 (95% CI 0.87-0.93) in predicting amyloid PET status (measuring 11C-PIB-PET, florbetapir or florbetaben) in 414 participants from 6 cohorts (91).
A validation study using pooled data from 2 independent cohorts (total N=686; MCI or mild dementia, n=378) was performed to evaluate the performance of PrecivityAD in identifying amyloid PET status (measured using florbetapir, florbetaben or flutemetamol) (92). Based on Aβ42/40 ratio, age and ApoE the PrecivityAD APS demonstrated an AUC of 0.88 (95% CI 0.85-0.91). To improve both the NPV and PPV, the authors identified a lower cutoff (low APS 0-35) and an upper cutoff (high APS 58-100); the resultant intermediate APS range was 36-57 (95 participants [14%] fell in the intermediate APS range). Reweighting for a population with a 60% prevalence of amyloid PET positivity, a low APS demonstrated a NPV of 86% while a high APS demonstrated a PPV of 86%. Diagnostic performance analyses showed that excluding individuals with an intermediate APS score, the APS showed 92% PPA, 77% NPA, and 85% accuracy in predicting amyloid PET positivity. Considering those with an intermediate score as positive resulted in a 93% PPA, 65% NPA and 80% accuracy, while considering these individuals as negative the PPA, NPA and accuracy were 80%. Of note, with the PrecivityAD2™ (under development) (93), amyloid status will be based on a binary determination (positive or negative) rather than be considered low, intermediate or high APS.
→ PrecivityAD™ is CE marked in EU (94).
→ PrecivityAD™ is available as LDT for clinical use and has FDA BDD in the US (95).
ABtest-IA (Araclon Biotech [a subsidiary of Grifols], Zaragoza, Spain) – ELISA
The performance of an ELISA-based total plasma Aβ42/40 ratio assay was recently evaluated in a subset of samples from the Australian Imaging, Biomarkers and Lifestyle (AIBL) study (96). Samples were collected at 3 timepoints (18, 36 and 54 months; N=176, 169 and 135, respectively). Using 11C-PiB-PET positivity at quantification as the SoT and a threshold defined using the Youden method, the total plasma Aβ42/40 ratio agreement with 11C-PiB-PET status demonstrated 63-65% OPAs, 68-76% PPAs and 53-62% NPAs across timepoints. Adjusting for age, sex, ApoE status and clinical classification, the ABtest-IA plasma Aβ42/40 ratio assay showed improved performances, with 83-85% OPAs, 0.88-0.91 AUCs, 83% PPA, and 84-86% NPAs across the 3 timepoints. In a study of 59 participants (MCI, n=20; CN, n=39), the total plasma Aβ42/40 ratio (Aβ42 and Aβ40 measured with ELISA kits from Araclon Biotech) was compared with 11C-PIB-PET findings; the total plasma Aβ42/40 ratio showed an AUC of 0.88 (95% CI 0.78-0.98) in predicting amyloid PET status, with 78% PPA and 88% NPA (97).
ABtest-MS (based on liquid chromatography coupled to mass spectrometry) has also been developed by Araclon for quantification of Aβ42 and Aβ40 (85).
→ ABtest-IA and ABtest-MS are CE marked in EU (84, 85).
Quest AD-detect™ (Quest Diagnostics, Secaucus, NJ) – LC-MS/MS
In company provided documentation (98) and in a recent abstract presented at AAIC 2022 (99), Quest AD-detect showed an AUC of 0.86, a PPA of 71% and an NPA of 89% in predicting amyloid PET status in a cohort (N=209) of individuals with AD, MCI or CN.
→ Quest AD-detect™ is available as LDT for clinical use in the US (100).
Automated Immunoassay System HISCL™-5000/HISCL™-800 (Sysmex, Kobe, Japan) – CLEIA
The performance of the plasma Aβ42/40 ratio measured using the Sysmex automated immunoassay platform (HISCL series) was recently evaluated in 2 study cohorts (N=197 and N=200) with MCI or mild dementia due to AD (101). Amyloid PET (performed using 3 regulatory approved radioligands) with visual read was used as a SoT. For the 2 study cohorts, AUCs were 0.94 and 0.87, respectively, with PPAs of 96% and 88% and NPAs of 84% and 72% based on thresholds maximizing the Youden Index. Using amyloid PET positivity at quantitation instead of visual read, AUCs were 0.93 and 0.92, respectively.
→ Sysmex Plasma Amyloid-β automated immunoassay system HISCL-5000/HISCL-800 is CE-marked in EU (102).
Tau Status
Plasma P-Tau181
P-tau181 (Quanterix, Billerica, MA) – Simoa®
A recent study of 200 participants (CN, N=177; MCI, N=23) evaluated the performance of the Quanterix plasma P-tau181 Simoa in predicting a tau PET status, established using flortaucipir PET and quantitation in both a region affected early in the disease process (entorhinal cortex) and in a region affected in more advanced disease (temporal composite region of interest [metaROI]) (103). Quanterix P-tau181 Simoa showed an AUC of 0.73 (95% CI 0.64-0.82) and 0.69 (95% CI 0.60-0.78) in the prediction of tau PET positivity in the entorhinal or temporal metaROIs, respectively.
→ Quanterix plasma P-tau181 SIMOA is available as an LDT for clinical use (104) and has FDA BDD in the US (105).
Relationships between PET, CSF and blood-based biomarkers
PET- and CSF-based amyloid and tau measures are widely considered valid biomarkers for ascertaining the presence or absence of ongoing AD pathology in symptomatic patients (50) as is evident from their mutual inclusion in the most updated clinical criteria (7, 20) and in the ATN research framework (6). CSF-based biomarkers, together with PET, are also included in the recent Alzheimer’s Association appropriate use recommendations as a SoT against which blood-based biomarker performances can be assessed s (106).
The temporal trajectories of these biomarkers do, however, differ (107, 108). Current models postulate that, as disease progresses, changes are first detected in fluid-based (CSF or blood) Aβ biomarkers and, subsequently, abnormal amyloid PET findings are detectable (AD cascade model) (107). This temporal difference is likely reflective of the differences in proteins measured; soluble and diffusible Aβ fractions (reflecting production/clearance at time of blood draw/lumbar puncture) are measured by fluid-based biomarkers while PET measures aggregated Aβ (109). In line with this, individuals with CSF Aβ positivity are more likely to show increased amyloid PET binding at follow-up (110, 111). Subsequent to Aβ aggregation, there is increased secretion of P-tau, which can be detected in CSF and/or plasma; this is followed by of NFT formation, detected by tau PET (15, 88).
The differing temporal trajectories of biomarkers, outlined above, have several implications for the interpretation of correlation data and for the utilization of these biomarkers (in terms of their ability to be used interchangeably) in clinical and research settings. Importantly, a binary concordance (positive/positive or negative/negative) across amyloid/tau fluid and PET biomarkers would be expected to increase with progression of symptomatic disease, thus showing highest concordance in individuals with advanced objective cognitive impairment due to AD pathology (110, 112).
In the case of Aβ detection, one should keep in mind that the quantitative relationship between amyloid PET and fluid-based Aβ biomarker findings is not linear, with fluid biomarkers being more sensitive to early Aβ changes, and PET biomarkers more sensitive to Aβ plaque deposition over the disease course. Amyloid PET negativity can correspond to a wide range of fluid-based Aβ concentrations; similarly, fluid-based Aβ positivity can correspond to a wide range of levels of amyloid PET radiotracer neocortical binding (113, 114). The relationship between tau PET binding and CSF P-tau concentration is believed to be more linear than in the case of amyloid PET/fluid-based Aβ biomarkers; however, one similarity is that a given CSF P-tau value can correspond to a range of levels of tau PET radiotracer neocortical binding (115). The magnitude of the association is impacted by several factors including population (e.g., early versus late disease phase), fluid analysis assay/platform and tau-PET acquisition/quantitation approaches.
Predicting amyloid/tau status through tau/amyloid biomarker findings
While the ATN framework requires concurrent presence of amyloid (A+) and tau (T+) for a diagnosis of AD, several lines of evidence indicate that their inter-relationship is also significant and potentially informative. In the context of PET-based biomarkers, for example, flortaucipir-PET positivity (an indicator of T+ in the ATN classification) is almost exclusively observed in individuals who also show amyloid positivity (116). These findings based on PET-based AD pathology evaluation are consistent with those from postmortem studies in which Braak V/VI at autopsy was almost exclusively observed in brains showing moderate-to-frequent neuritic plaque density (117). Additionally, several fluid-based tau biomarker assays have been validated against amyloid PET, and this is consistent with the temporal trajectory of the biomarkers. While more studies are needed, these observations provide some evidence that flortaucipir PET positivity, ascertained using specific criteria and methodology, could be a robust indicator of both T+ and A+ status. However, the converse is not necessarily the case; while A- status would be highly indicative of T- status, A+ status alone is not per se indicative of T+ status nor is T- status per se indicative of A- status.
In the context of CSF-based biomarkers, several studies have reported that assays to detect both amyloid and tau (e.g., P-tau181/Aβ42 or T-tau/Aβ42 ratios) perform well, and sometimes better than tests for amyloid or tau individually (54, 69, 70) in predicting AD pathology at autopsy or amyloid PET SoTs (61-64, 75, 76, 118). Overall, these data suggest that there is value in considering both amyloid and tau CSF marker findings when predicting amyloid status as defined by PET. In the case of blood-based biomarkers, studies are needed to evaluate the performance of plasma tau biomarkers (e.g., plasma P-tau181) in the prediction of both amyloid and tau PET status (103).
Discussion
While numerous diagnostic tests are available, their use in clinical practice in the AD field is limited (17). It is likely that the complexity of the AD biomarker field is partly responsible for this. This review provides an overview of diagnostic tests and their performance to help clinicians with optimal management of their patients with cognitive or behavioral symptoms. We review published findings on the ability of PET, CSF and blood-based assays that are authorized in the US or EU or run as LDTs in the US to ascertain amyloid and tau status in the US and/or EU; these assays are summarized in Table 2 and tabulated in more detail in the supplementary table. It is recognized that authorization by a regulatory authority does not necessarily equate to availability to HCP; accessibility will be dependent on many factors, including availability of necessary resources (imaging tools) and reimbursement options.
In defining amyloid status using PET, all approved radiotracers performed well in predicting amyloid pathology at autopsy. CSF-based biomarkers, validated with either autopsy- or PET-based amyloid pathology confirmation, showed similar performance across products and manufacturers, although the CSF Aβ42/40 and P-tau181/Aβ42 concentration ratios generally outperformed the CSF Aβ42 or P-tau181 concentrations alone. All available tau biomarker assays accurately predicted tau pathology as measured at autopsy or using tau PET.
Findings to date support the interchangeable use of PET or fluid-based biomarkers to determine positivity in symptomatic participants; however, as a result of their non-linear quantitative relationship, this may not be appropriate in the preclinical stage of disease. For example, individuals with the same CSF Aβ42 concentration could exhibit varying degrees of neocortical amyloid PET binding.
In recent years, development of fluid-based biomarkers has accelerated. This is the result of the ability to use validated PET, rather than autopsy, to evaluate their performance and the increased accessibility to PET. In the US, the only FDA-authorized fluid-based biomarker assays to be used as an aid in the diagnosis of AD were developed under the BDD program; the FDA has granted BDD to multiple fluid-based biomarker assays, reflecting an intent to expedite development of these promising biomarker tests. Fluid-based biomarker development continues to advance through the use of fully automated assays that offer improved test reliability as well as less variability across laboratories. We refer the reader to the respective labels for further information related to calibration and determining assay thresholds.
Novel biomarkers based on plasma P-tau181 or P-tau217 are at various stages of development. Preliminary data show these biomarkers to have high accuracy in predicting both amyloid and tau status, as defined by CSF-, PET- or autopsy-based evidence and they have started to be used, and further tested, in clinical trials as pre-screening or screening tools for patient eligibility (93, 103, 106, 119, 120). The FDA has granted BDD to 2 tests based on the plasma P-tau181 biomarker. While promising in terms of costs and accessibility for clinical practice, these biomarkers require thorough technical validation and standardization, as well as prospective testing in more diverse populations, including evaluation of the possible impact of comorbid conditions on test performance (106, 119). Ongoing studies are also evaluating the ability of CSF and plasma tau biomarkers to predict amyloid status. While promising from a research perspective, commercially available tests in clinical practice settings should be used in line with current label indications.
While the focus of this review is the clinical validation of biomarkers, ultimately the biomarkers need to be employed appropriately and exhibit value in clinical practice. There has been a significant effort to create recommendations for use of amyloid PET in clinical practice (121-123). Moreover, findings from large studies such as the US-based Imaging Dementia – Evidence for Amyloid Scanning (IDEAS) study and the EU-based Amyloid Imaging to Prevent Alzheimer’s Disease (AMYPAD) Diagnostic and Patient Management study have demonstrated significant impact of the use of amyloid PET on outcomes such as diagnostic change, diagnostic confidence and patient management (124, 125), with smaller studies providing supporting evidence (126, 127). In the case of tau PET, with only a single radioligand currently approved for clinical use (in the US), there have been initial efforts in this realm (128), but more work is needed to devise clinical guidelines. Use of flortaucipir, as well as unapproved tau PET radioligands, has been shown to a significant impact on diagnostic change and confidence, similar to that seen with amyloid PET (129, 130). In the case of CSF and blood-based biomarkers, criteria and recommendations for use, respectively, have been published (106, 131, 132). Recent findings from a meta-analysis of published studies on the clinical utility of CSF biomarkers demonstrated their value as a diagnostic tool (133); studies are currently ongoing to evaluate the clinical impact of blood-based biomarkers (e.g. the Quality Improvement PrecivityAD Clinician Survey [QUIP I]) (134).
There are several limitations to this review. First, it was not intended to be a comprehensive review of all available evidence but an overview to help clinicians navigate key performance data on diagnostic tests that are authorized in the US or EU or available as LDTs in the US. We performed a targeted search of commercially available biomarkers as of August 2022, prioritizing studies where there was either autopsy- or PET-based pathology confirmation. For CSF biomarkers, unless described as part of the company assay documentation, we generally excluded studies where assay performance was assessed through their ability to differentiate between individuals clinically diagnosed with AD and those with non-AD conditions or no cognitive impairment; this topic is reviewed elsewhere (48, 49). A systematic literature review of biomarker assays that considers all performance studies, and the associated heterogeneity in methodology, would certainly be of value in helping HCPs to definitively compare assay performance. Second, as a result of the rapidly evolving biomarker landscape the list of approved diagnostic tests included in this review may not be exhaustive. Third, while challenges in AD diagnosis are of global concern, our review focused solely on the US and EU landscapes in part to simplify this already complex topic and in part due to limited access to biomarker assays and information in many countries. Finally, while the EU landscape was a primary focus for this paper, we did not consider EU country-specific variations in regulations and reimbursement.
In conclusion, a number of PET- and fluid-based biomarkers for the detection of both amyloid and tau pathologies are now available for use in the US and EU. All assays generally accurately detect amyloid or tau pathology in populations with AD, though there is some variability in performance findings dependent on methodological differences. Importantly, assays should be employed in accordance with label indication and recommendation. In some cases, further validation efforts may be needed, and this will ultimately help control pre-analytical, analytical, and post-analytical sources of variability; this standardization will help define thresholds that can be applied across centers and geographies, facilitating broad adoption and informed use by HCPs.
Funding: See conflicts of interest.
Acknowledgements: We are grateful to Jim Hendrix, Michelle Neff, Simona Vasileva, Rachael Wisler Keller and Gregg Mayer for their invaluable contribution to this review – for input on scientific content (Hendrix, Vasileva), and navigation of the regulatory environment (M Neff) and biomarker landscape (Wisler Keller, Mayer).
Conflict of interest: All authors are full time employees and minor stockholders at Eli Lilly and Company.
Open Access: This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits use, duplication, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license and indicate if changes were made.
References
1. Jack CR, Knopman DS, Jagust WJ, et al. Tracking pathophysiological processes in Alzheimer’s disease: an updated hypothetical model of dynamic biomarkers. Lancet Neurol 2013;12:207-216.
2. Bateman RJ, Xiong C, Benzinger T, et al. Clinical and biomarker changes in dominantly inherited Alzheimer’s disease. N Engl J Med 2012;367:795-804.
3. Villemagne VL, Burnham S, Bourgeat P, et al. Amyloid β deposition, neurodegeneration, and cognitive decline in sporadic Alzheimer’s disease: a prospective cohort study. Lancet Neurol 2013;12:357-367.
4. Beach TG, Monsell SE, Phillips LE, Kukull W. Accuracy of the clinical diagnosis of Alzheimer disease at National Institute on Aging Alzheimer Disease Centers, 2005–2010. J Neuropathol Exp Neurol 2012;71:266-273.
5. Jack CR, Bennett DA, Blennow K, et al. A/T/N: An unbiased descriptive classification scheme for Alzheimer disease biomarkers. Neurology 2016;87:539-547.
6. Jack Jr CR, Bennett DA, Blennow K, et al. NIA-AA research framework: toward a biological definition of Alzheimer’s disease. Alzheimers Dement 2018;14:535-562.
7. Dubois B, Villain N, Frisoni GB, et al. Clinical diagnosis of Alzheimer’s disease: recommendations of the International Working Group. Lancet Neurol 2021;20:484-496.
8. Mintun MA, Lo AC, Duggan Evans C, et al. Donanemab in early Alzheimer’s disease. N Engl J Med 2021;384:1691-1704. DOI: doi: 10.1056/NEJMoa2100708.
9. Budd Haeberlein S, Aisen P, Barkhof F, et al. Two randomized phase 3 studies of aducanumab in early Alzheimer’s disease. J Prev Alzheimers Dis 2022;9:197-210.
10. van Dyck CH, Swanson CJ, Aisen P, et al. Lecanemab in early Alzheimer’s disease. N Engl J Med 2022 2022/12/01. DOI: 10.1056/NEJMoa2212948.
11. Bateman R, Smith J, Donohue M, et al. Topline results of Phase 3 GRADUATE I & II pivotal trials with subcutaneous gantenerumab J Prev Alzheimer’s Dis 2023;9:60.
12. Clark CM, Pontecorvo MJ, Beach TG, et al. Cerebral PET with florbetapir compared with neuropathology at autopsy for detection of neuritic amyloid-β plaques: a prospective cohort study. Lancet Neurol 2012;11:669-678.
13. Sabri O, Sabbagh MN, Seibyl J, et al. Florbetaben PET imaging to detect amyloid beta plaques in Alzheimer’s disease: phase 3 study. Alzheimers Dement 2015;11:964-974.
14. Curtis C, Gamez JE, Singh U, et al. Phase 3 trial of flutemetamol labeled with radioactive fluorine 18 imaging and neuritic plaque density. JAMA Neurol 2015;72:287-294.
15. Fleisher AS, Pontecorvo MJ, Devous MD, et al. Positron emission tomography imaging with [18F] flortaucipir and postmortem assessment of Alzheimer disease neuropathologic changes. JAMA Neurol 2020;77:829-839.
16. Epelbaum S, Paquet C, Hugon J, et al. How many patients are eligible for disease-modifying treatment in Alzheimer’s disease? A French national observational study over 5 years. BMJ Open 2019;9:e029663.
17. Caprioglio C, Garibotto V, Jessen F, et al. The clinical use of Alzheimer’s disease biomarkers in patients with mild cognitive impairment: A European Alzheimer’s disease consortium survey. J Alzheimers Dis;89:535-551.
18. Hampel H, Shaw LM, Aisen P, et al. State-of-the-art of lumbar puncture and its place in the journey of patients with Alzheimer’s disease. Alzheimers Dement 2022;18:159-177.
19. Dubois B, Feldman HH, Jacova C, et al. Revising the definition of Alzheimer’s disease: a new lexicon. Lancet Neurol 2010;9:1118-1127.
20. McKhann GM, Knopman DS, Chertkow H, et al. The diagnosis of dementia due to Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement 2011;7:263-269.
21. Albert MS, DeKosky ST, Dickson D, et al. The diagnosis of mild cognitive impairment due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement 2011;7:270-279.
22. Sperling RA, Aisen PS, Beckett LA, et al. Toward defining the preclinical stages of Alzheimer’s disease: Recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement 2011;7:280-292.
23. Dubois B, Feldman HH, Jacova C, et al. “Advancing research diagnostic criteria for Alzheimer’s disease: The IWG-2 criteria.”: Correction. 2014;13:757.
24. Dubois B, Feldman HH, Jacova C, et al. Research criteria for the diagnosis of Alzheimer’s disease: revising the NINCDS–ADRDA criteria. Lancet Neurol 2007;6:734-746.
25. Villemagne VL, Doré V, Burnham SC, Masters CL, Rowe CC. Imaging tau and amyloid-β proteinopathies in Alzheimer disease and other conditions. Nat Rev Neurol 2018;14:225-236.
26. Pemberton HG, Collij LE, Heeman F, et al. Quantification of amyloid PET for future clinical use: a state-of-the-art review. Eur J Nucl Med Mol Imaging 2022:3508-35281.
27. Klunk WE, Koeppe RA, Price JC, et al. The Centiloid Project: standardizing quantitative amyloid plaque estimation by PET. Alzheimers Dement 2015;11:1-15.e11-14. 2014/12/03. DOI: 10.1016/j.jalz.2014.07.003.
28. Amyvid® (florbetapir F 18 injection) [package insert]. Eli Lilly and Company, Indianapolis, IN; 2019. https://pi.lilly.com/us/amyvid-uspi.pdf?s=pi Accessed Aug 2022.
29. Amyvid® (florbetapir F 18 injection) [product information]. Eli Lilly Nederland B.V, Urtrecht, The Netherlands; 2019. https://www.ema.europa.eu/en/documents/product-information/amyvid-epar-product-information_en.pdf Accessed Aug 2022.
30. Beach TG, Maarouf CL, Intorcia A, et al. Antemortem-postmortem correlation of florbetapir (18F) PET amyloid imaging with quantitative biochemical measures of Aβ 42 but not Aβ 40. J Alzheimers Dis 2018;61:1509-1516.
31. Teipel SJ, Temp AG, Levin F, et al. Association of PET-based stages of amyloid deposition with neuropathological markers of Aβ pathology. Ann Clin Transl Neurol 2021;8:29-42.
32. Neuraceq® (florbetaben F 18 injection) [package insert]. Life Molecular Imaging Ltd, Warwick, UK; 2021. https://neuraceq.com/wp-content/uploads/2022/09/PRESCRIBING-INFORMATION.pdf Accessed Aug 2022.
33. Neuraceq® (florbetaben F 18 injection) [product information]. Life Radiopharma, Berlin GmbH, Germany; 2019. https://www.ema.europa.eu/en/documents/product-information/neuraceq-epar-product-information_en.pdf Accessed Aug 2022.
34. Doré V, Bullich S, Rowe CC, et al. Comparison of 18F-florbetaben quantification results using the standard Centiloid, MR-based, and MR-less CapAIBL® approaches: Validation against histopathology. Alzheimers Dement 2019;15:807-816.
35. Bullich S, Seibyl J, Catafau AM, et al. Optimized classification of 18F-Florbetaben PET scans as positive and negative using an SUVR quantitative approach and comparison to visual assessment. Neuroimage Clin 2017;15:325-332.
36. VizamylTM (flutemetamol F 18 injection) [product information]. GE Healthcare AS, Oslo, Norway; 2019. https://www.ema.europa.eu/en/documents/product-information/vizamyl-epar-product-information_en.pdf Accessed Aug 2022.
37. VizamylTM (flutemetamol F 18 injection) [package insert]. GE Healthcare, Arlington Heights, IL; 2020. https://www.gehealthcare.com/-/jssmedia/widen/2018/01/25/0204/gehealthcarecom/migrated/2018/02/19/0834/er-clinical-product-info-vizamyl-203-8c17d992a0aa9aadb2e446d7f5580a8b_43-1067c_vizamyl_pdf.pdf?la=en-usAccessed Aug 2022.
38. Thal DR, Beach TG, Zanette M, et al. [18F] flutemetamol amyloid positron emission tomography in preclinical and symptomatic Alzheimer’s disease: specific detection of advanced phases of amyloid-β pathology. Alzheimers Dement 2015;11:975-985.
39. Ikonomovic MD, Buckley CJ, Heurling K, et al. Post-mortem histopathology underlying β-amyloid PET imaging following flutemetamol F 18 injection. Acta Neuropathol Commun 2016;4:1-24.
40. Salloway S, Gamez JE, Singh U, et al. Performance of [18F] flutemetamol amyloid imaging against the neuritic plaque component of CERAD and the current (2012) NIA-AA recommendations for the neuropathologic diagnosis of Alzheimer’s disease. Alzheimers Dement (Amst) 2017;9:25-34.
41. Collij LE, Salvadó G, Shekari M, et al. Visual assessment of [18F] flutemetamol PET images can detect early amyloid pathology and grade its extent. Eur J Nucl Med Mol Imaging 2021;48:2169-2182.
42. TAUVIDTM (flortaucipir F 18 injection) [package insert]. Eli Lilly and Company, Indianapolis, IN; 2022. https://pi.lilly.com/us/tauvid-uspi.pdf Accessed Aug 2022.
43. Josephs KA, Tosakulwong N, Gatto RG, et al. Optimum differentiation of frontotemporal lobar degeneration from Alzheimer disease achieved with cross-sectional tau positron emission tomography. Ann Neurol 2022;92:1016-1029.
44. Soleimani-Meigooni DN, Iaccarino L, La Joie R, et al. 18F-flortaucipir PET to autopsy comparisons in Alzheimer’s disease and other neurodegenerative diseases. Brain 2020;143:3477-3494.
45. Lowe VJ, Lundt ES, Albertson SM, et al. Tau-positron emission tomography correlates with neuropathology findings. Alzheimers Dement 2020;16:561-571.
46. Pontecorvo MJ, Keene CD, Beach TG, et al. Comparison of regional flortaucipir PET with quantitative tau immunohistochemistry in three subjects with Alzheimer’s disease pathology: a clinicopathological study. EJNMMI Res 2020;10:65.
47. Smith R, Wibom M, Pawlik D, Englund E, Hansson O. Correlation of in vivo [18F] flortaucipir with postmortem Alzheimer disease tau pathology. JAMA Neurol 2019;76:310-317.
48. Olsson B, Lautner R, Andreasson U, et al. CSF and blood biomarkers for the diagnosis of Alzheimer’s disease: a systematic review and meta-analysis. Lancet Neurol 2016;15:673-684.
49. Hazan J, Wing M, Liu KY, Reeves S, Howard R. Clinical utility of cerebrospinal fluid biomarkers in the evaluation of cognitive impairment: a systematic review and meta-analysis. J Neurol Neurosurg Psychiatry 2022;jnnp-2022-329530.
50. Hampel H, Au R, Mattke S, et al. Designing the next-generation clinical care pathway for Alzheimer’s disease. Nat Aging 2022;2:692-703.
51. Zetterberg H, Blennow K. Moving fluid biomarkers for Alzheimer’s disease from research tools to routine clinical diagnostics. Mol Neurodegener 2021;16:1-7.
52. Hansson O, Lehmann S, Otto M, Zetterberg H, Lewczuk P. Advantages and disadvantages of the use of the CSF Amyloid β (Aβ) 42/40 ratio in the diagnosis of Alzheimer’s disease. Alzheimers Res Ther 2019;11:34.
53. Bouwman FH, Frisoni GB, Johnson SC, et al. Clinical application of CSF biomarkers for Alzheimer’s disease: From rationale to ratios. Alzheimers Dement (Amst) 2022;14:e12314.
54. Tapiola T, Alafuzoff I, Herukka S-K, et al. Cerebrospinal fluid β-amyloid 42 and tau proteins as biomarkers of Alzheimer-type pathologic changes in the brain. Arch Neurol 2009;66:382-389.
55. Strozyk D, Blennow K, White L, Launer L. CSF Abeta 42 levels correlate with amyloid-neuropathology in a population-based autopsy study. Neurology 2003;60:652-656.
56. Seppälä T, Nerg O, Koivisto A, et al. CSF biomarkers for Alzheimer disease correlate with cortical brain biopsy findings. Neurology 2012;78:1568-1575.
57. Bridel C, Somers C, Sieben A, et al. Associating Alzheimer’s disease pathology with its cerebrospinal fluid biomarkers. Brain 2022;145:4056-4064.
58. Reimand J, Boon B, Collij LE, et al. Amyloid-β PET and CSF in an autopsy-confirmed cohort. Ann Clin Transl Neurol 2020;7:2150-2160.
59. Schoonenboom NS, Reesink FE, Verwey NA, et al. Cerebrospinal fluid markers for differential dementia diagnosis in a large memory clinic cohort. Neurology 2012;78:47-54. 2011/12/16. DOI: 10.1212/WNL.0b013e31823ed0f0.
60. Request information at Fujirebio website. https://www.fujirebio.com/ Accessed Aug 2022.
61. Alcolea D, Pegueroles J, Munoz L, et al. Agreement of amyloid PET and CSF biomarkers for Alzheimer’s disease on Lumipulse. Ann Clin Transl Neurol 2019;6:1815-1824.
62. Kaplow J, Vandijck M, Gray J, et al. Concordance of Lumipulse cerebrospinal fluid t-tau/Aβ42 ratio with amyloid PET status. Alzheimers Dement 2020;16:144-152.
63. Moon S, Kim S, Mankhong S, et al. Alzheimer’s cerebrospinal biomarkers from Lumipulse fully automated immunoassay: concordance with amyloid-beta PET and manual immunoassay in Koreans: CSF AD biomarkers measured by Lumipulse in Koreans. Alzheimers Res Ther 2021;13:22.
64. Campbell MR, Ashrafzadeh-Kian S, Petersen RC, et al. P-tau/Aβ42 and Aβ42/40 ratios in CSF are equally predictive of amyloid PET status. Alzheimers Dement (Amst) 2021;13:e12190.
65. Willemse EA, Tijms BM, van Berckel BN, et al. Comparing CSF amyloid-beta biomarker ratios for two automated immunoassays, Elecsys and Lumipulse, with amyloid PET status. Alzheimers Dement (Amst) 2021;13:e12182.
66. Sacchi L, Carandini T, Fumagalli GG, et al. Unravelling the association between amyloid-PET and cerebrospinal fluid biomarkers in the Alzheimer’s disease spectrum: Who really deserves an A+? . J Alzheimers Dis 2022;85:1009-1020.
67. Lumipulse G β-Amyloid Ratio (1-42/1-40). US Sales Sheet. Fujirebio, Tokyo, Japan. https://www.fujirebio.com/sites/default/files/2022-07/lumipulse_g_b-amyloid_ratio_1-42-1-40_sales_sheet.pdf Accessed Aug 2022.
68. Fujirebio News and Events Feb 14 2019. https://www.fujirebio.com/en-us/news-events/fujirebio-diagnostics-receives-fda-breakthrough-device-designation-for-lumipulser-g Accessed Aug 2022.
69. Mattsson-Carlgren N, Grinberg LT, Boxer A, et al. Cerebrospinal fluid biomarkers in autopsy-confirmed Alzheimer disease and frontotemporal lobar degeneration. Neurology 2022;98:e1137-e1150.
70. Grothe MJ, Moscoso A, Ashton NJ, et al. Associations of fully automated CSF and novel plasma biomarkers with Alzheimer disease neuropathology at autopsy. Neurology 2021;97:e1229-e1242.
71. Elecsys β-Amyloid (1-42) CSF II – Ref 08821941190 [Instructions for use]. Roche Diagnostics, Rotkreuz, Switzerland 2021. https://pim-eservices.roche.com/eLD/api/downloads/7aa19107-2bbd-eb11-0391-005056a772fd?countryIsoCode=ie Accessed Aug 2022.
72. Roche Investor Updates Jul 20 2018. https://www.roche.com/investors/updates/inv-update-2018-07-20 Accessed Aug 2022.
73. Elecsys Phospho-Tau (181P) CSF – Ref 07357036 190 [Instructions for use]. Roche Diagnostics, Rotkreuz, Switzerland 2021. https://pim-eservices.roche.com/eLD/api/downloads/885e3b12-18df-eb11-0b91-005056a71a5d?countryIsoCode=pi Accessed Aug 2022.
74. Janelidze S, Zetterberg H, Mattsson N, et al. CSF Aβ42/Aβ40 and Aβ42/Aβ38 ratios: better diagnostic markers of Alzheimer disease. Ann Clin Transl Neurol 2016;3:154-165.
75. Janelidze S, Pannee J, Mikulskis A, et al. Concordance between different amyloid immunoassays and visual amyloid positron emission tomographic assessment. JAMA Neurol 2017;74:1492-1501.
76. Álvarez I, Diez-Fairen M, Aguilar M, et al. Added value of cerebrospinal fluid multimarker analysis in diagnosis and progression of dementia. Eur J Neurol 2021;28:1142-1152.
77. Janelidze S, Mattsson N, Palmqvist S, et al. Plasma P-tau181 in Alzheimer’s disease: relationship to other biomarkers, differential diagnosis, neuropathology and longitudinal progression to Alzheimer’s dementia. Nat Med 2020;26:379-386.
78. Mattsson-Carlgren N, Leuzy A, Janelidze S, et al. The implications of different approaches to define AT (N) in Alzheimer disease. Neurology 2020;94:e2233-e2244.
79. Request information at Euroimmun website. https://www.euroimmun.com/ Accessed Aug 2022.
80. Lewczuk P, Matzen A, Blennow K, et al. Cerebrospinal fluid Aβ 42/40 corresponds better than Aβ 42 to amyloid PET in Alzheimer’s disease. J Alzheimers Dis 2017;55:813-822.
81. Request information at TECAN website. https://www.ibl-international.com/ Accessed Aug 2022.
82. TECAN Phospho-TAU ELISA – Ref 30121609 [Instructions for use]. IBL International, Hamburg, Germany 2019. https://www.ibl-international.com/media/mageworx/downloads/attachment/file/3/0/30121609_ifu_eu_en_phosphotau_elisa_v10_2020_7.pdf Accessed Aug 2022.
83. Amyloid-beta (1-42) CSF ELISA – Ref RE59661 [Instructions for use]. IBL International, Hamburg, Germany 2015. https://www.ibl-international.com/media/mageworx/downloads/attachment/file/r/e/re59661_ifu_us_en_amyloid-beta__1-42__csf_elisa_2019-05_sym4.pdf Accessed Aug 2022.
84. Request information at Araclon Biotec [ABtest-IA page]. https://www.araclon.com/en/abtest-ia-2/ Accessed Aug 2022.
85. Grifols Newsroom Sept 20, 2022. https://www.grifols.com/en/view-news/-/news/araclon-biotech-obtains-ce-mark-for-early-stage-alzheimer-s-disease-diagnostic-tests Accessed Oct 2022.
86. Tariciotti L, Casadei M, Honig LS, et al. Clinical Experience with Cerebrospinal Fluid Aβ42, Total and Phosphorylated Tau in the Evaluation of 1,016 Individuals for Suspected Dementia. J Alzheimers Dis 2018;65:1417-1425. 2018/08/29. DOI: 10.3233/jad-180548.
87. Request information at Athena Diagnostics website. https://www.athenadiagnostics.com/ Accessed Feb 2023.
88. Mattsson-Carlgren N, Andersson E, Janelidze S, et al. Aβ deposition is associated with increases in soluble and phosphorylated tau that precede a positive Tau PET in Alzheimer’s disease. Sci Adv 2020;6:eaaz2387.
89. Montine TJ, Phelps CH, Beach TG, et al. National Institute on Aging–Alzheimer’s Association guidelines for the neuropathologic assessment of Alzheimer’s disease: a practical approach. Acta Neuropathol 2012;123:1-11.
90. Pannee J, Shaw LM, Korecka M, et al. The global Alzheimer’s Association round robin study on plasma amyloid β methods. Alzheimers Dement (Amst) 2021;13:e12242.
91. West T, Kirmess KM, Meyer MR, et al. A blood-based diagnostic test incorporating plasma Aβ42/40 ratio, ApoE proteotype, and age accurately identifies brain amyloid status: findings from a multi cohort validity analysis. Mol Neurodegener 2021;16:30.
92. Hu Y, Kirmess KM, Meyer MR, et al. Assessment of a plasma amyloid probability score to estimate amyloid positron emission tomography findings among adults with cognitive impairment. JAMA Netw Open 2022;5:e228392-e228392.
93. C₂N Diagnostics Introduces the PrecivityAD2™ Blood Test. https://precivityad.com/news/c2n-diagnostics-introduces-the-precivityad2-blood-test Accessed Feb 2023.
94. Request information at PrecivityADTM website. https://precivityad.com/ Accessed Aug 2022.
95. C2N News Release Jan 29 2019. https://c2n.com/news-releases/2019/01/29/2019-1-24-c2n-diagnostics-receives-breakthrough-device-designation-from-us-fda-for-blood-test-to-screen-for-alzheimers-disease-risk Accessed Aug 2022.
96. Doecke JD, Pérez-Grijalba V, Fandos N, et al. Total Aβ42/Aβ40 ratio in plasma predicts amyloid-PET status, independent of clinical AD diagnosis. Neurology 2020;94:e1580-e1591.
97. Pérez-Grijalba V, Arbizu J, Romero J, et al. Plasma Aβ42/40 ratio alone or combined with FDG-PET can accurately predict amyloid-PET positivity: a cross-sectional analysis from the AB255 Study. Alzheimers Res Ther 2019;11:96.
98. Quest AD-Detect, Beta-Amyloid 42/40 Ratio, Plasma. https://testdirectory.questdiagnostics.com/test/test-guides/TS_AD_Detect_BetaRatioPlasma/quest-ad-detect-beta-amyloid-4240-ratio-plasmas Accessed Aug 2022.
99. Edler MC, Russ KA, Mitchell CM, et al. A new LC-MS/MS assay for the quantification of Aβ40 and Aβ42 in plasma: validation and clinical performance. Presented at AAIC 2022. https://alz.confex.com/alz/2022/meetingapp.cgi/Paper/64182 Accessed Aug 2022.
100. Request information at Quest Diagnostics website. https://www.questdiagnostics.com/ Accessed Aug 2022.
101. Yamashita K, Miura M, Watanabe S, et al. Fully automated and highly specific plasma β-amyloid immunoassays predict β-amyloid status defined by amyloid positron emission tomography with high accuracy. Alzheimers Res Ther 2022;14:86. 2022/06/24. DOI: 10.1186/s13195-022-01029-0.
102. Sysmex News Release Jun 27 2022. https://www.sysmex.co.jp/en/news/2022/pdf/220627.pdf Accessed Feb 2023.
103. Mielke MM, Frank RD, Dage JL, et al. Comparison of plasma phosphorylated tau species with amyloid and tau positron emission tomography, neurodegeneration, vascular pathology, and cognitive outcomes. JAMA Neurol 2021;78:1108-1117.
104. Request information at Quanterix website. https://www.quanterix.com/ Accessed Aug 2022.
105. Quanterix Press Release Oct 11 2021. https://ir.quanterix.com/news-releases/news-release-details/quanterix-granted-breakthrough-device-designation-us-fda-blood Accessed Aug 2022.
106. Hansson O, Edelmayer RM, Boxer AL, et al. The Alzheimer’s Association appropriate use recommendations for blood biomarkers in Alzheimer’s disease. Alzheimers Dement 2022.
107. Hansson O. Biomarkers for neurodegenerative diseases. Nat Med 2021;27:954-963.
108. Guo Y, Huang Y-Y, Shen X-N, et al. Characterization of Alzheimer’s tau biomarker discordance using plasma, CSF, and PET. Alzheimers Res Ther 2021;13:93.
109. Roberts BR, Lind M, Wagen AZ, et al. Biochemically-defined pools of amyloid-β in sporadic Alzheimer’s disease: correlation with amyloid PET. Brain 2017;140:1486-1498.
110. Sala A, Nordberg A, Rodriguez-Vieitez E. Longitudinal pathways of cerebrospinal fluid and positron emission tomography biomarkers of amyloid-β positivity. Mol Psychiatry 2021;26:5864-5874.
111. Palmqvist S, Mattsson N, Hansson O, Initiative AsDN. Cerebrospinal fluid analysis detects cerebral amyloid-β accumulation earlier than positron emission tomography. Brain 2016;139:1226-1236.
112. Meyer P-F, Binette AP, Gonneaud J, et al. Characterization of Alzheimer disease biomarker discrepancies using cerebrospinal fluid phosphorylated tau and AV1451 positron emission tomography. JAMA Neurol 2020;77:508-516.
113. Toledo JB, Bjerke M, Da X, et al. Nonlinear association between cerebrospinal fluid and florbetapir F-18 β-amyloid measures across the spectrum of Alzheimer disease. JAMA Neurol 2015;72:571-581.
114. Salvadó G, Molinuevo JL, Brugulat-Serrat A, et al. Centiloid cut-off values for optimal agreement between PET and CSF core AD biomarkers. Alzheimers Res Ther 2019;11:27.
115. Janelidze S, Stomrud E, Smith R, et al. Cerebrospinal fluid p-tau217 performs better than p-tau181 as a biomarker of Alzheimer’s disease. Nat Commun 2020;11:1-12.
116. Ossenkoppele R, Hansson O. Towards clinical application of tau PET tracers for diagnosing dementia due to Alzheimer’s disease. Alzheimers Dement 2021;17:1998-2008.
117. Monsell SE, Mock C, Roe CM, et al. Comparison of symptomatic and asymptomatic persons with Alzheimer disease neuropathology. Neurology 2013;80:2121-2129.
118. Keshavan A, Wellington H, Chen Z, et al. Concordance of CSF measures of Alzheimer’s pathology with amyloid PET status in a preclinical cohort: A comparison of Lumipulse and established immunoassays. Alzheimers Dement (Amst) 2021;13:e12131.
119. Teunissen CE, Verberk IM, Thijssen EH, et al. Blood-based biomarkers for Alzheimer’s disease: towards clinical implementation. Lancet Neurol 2022;21:66-77.
120. Schindler SE, Li Y, Li M, et al. Using Alzheimer’s disease blood tests to accelerate clinical trial enrollment. Alzheimers Dement 2022.
121. Johnson KA, Minoshima S, Bohnen NI, et al. Appropriate use criteria for amyloid PET: a report of the Amyloid Imaging Task Force, the Society of Nuclear Medicine and Molecular Imaging, and the Alzheimer’s Association. J Nucl Med 2013;54:476-490. 2013/01/30. DOI: 10.2967/jnumed.113.120618.
122. Johnson KA, Minoshima S, Bohnen NI, et al. Update on appropriate use criteria for amyloid PET imaging: dementia experts, mild cognitive impairment, and education. J Nucl Med 2013;54:1011-1013. 2013/06/12. DOI: 10.2967/jnumed.113.127068.
123. Minoshima S, Drzezga AE, Barthel H, et al. SNMMI Procedure Standard/EANM Practice Guideline for Amyloid PET Imaging of the Brain 1.0. J Nucl Med 2016;57:1316-1322. 2016/08/03. DOI: 10.2967/jnumed.116.174615.
124. Rabinovici GD, Gatsonis C, Apgar C, et al. Association of Amyloid Positron Emission Tomography With Subsequent Change in Clinical Management Among Medicare Beneficiaries With Mild Cognitive Impairment or Dementia. Jama 2019;321:1286-1294. 2019/04/03. DOI: 10.1001/jama.2019.2000.
125. Altomare D, Barkhof F, Caprioglio C, et al. The use of amyloid-PET in memory clinic patients: AMYPAD Diagnostic and Patient Management Study. Annual Congress of the European Association of Nuclear Medicine October 15-19, 2022 Barcelona, Spain. European Journal of Nuclear Medicine and Molecular Imaging 2022;49:1-751. DOI: 10.1007/s00259-022-05924-4.
126. Fantoni ER, Chalkidou A, JT OB, Farrar G, Hammers A. A Systematic Review and Aggregated Analysis on the Impact of Amyloid PET Brain Imaging on the Diagnosis, Diagnostic Confidence, and Management of Patients being Evaluated for Alzheimer’s Disease. J Alzheimers Dis 2018;63:783-796. 2018/04/25. DOI: 10.3233/jad-171093.
127. Cotta Ramusino M, Perini G, Altomare D, et al. Outcomes of clinical utility in amyloid-PET studies: state of art and future perspectives. Eur J Nucl Med Mol Imaging 2021;48:2157-2168. 2021/02/18. DOI: 10.1007/s00259-020-05187-x.
128. Tian M, Civelek AC, Carrio I, et al. International consensus on the use of tau PET imaging agent (18)F-flortaucipir in Alzheimer’s disease. Eur J Nucl Med Mol Imaging 2022;49:895-904. 2022/01/04. DOI: 10.1007/s00259-021-05673-w.
129. Altomare D, Caprioglio C, Assal F, et al. Diagnostic value of amyloid-PET and tau-PET: a head-to-head comparison. Eur J Nucl Med Mol Imaging 2021;48:2200-2211. 2021/02/28. DOI: 10.1007/s00259-021-05246-x.
130. Shimohama S, Tezuka T, Takahata K, et al. Impact of Amyloid and Tau PET on Changes in Diagnosis and Patient Management. Neurology 2023;100:e264-e274. 2022/09/30. DOI: 10.1212/wnl.0000000000201389.
131. Shaw LM, Arias J, Blennow K, et al. Appropriate use criteria for lumbar puncture and cerebrospinal fluid testing in the diagnosis of Alzheimer’s disease. Alzheimers Dement 2018;14:1505-1521. 2018/10/15. DOI: 10.1016/j.jalz.2018.07.220.
132. Hansson O, Batrla R, Brix B, et al. The Alzheimer’s Association international guidelines for handling of cerebrospinal fluid for routine clinical measurements of amyloid β and tau. Alzheimers Dement 2021;17:1575-1582. 2021/04/01. DOI: 10.1002/alz.12316.
133. Hazan J, Wing M, Liu KY, Reeves S, Howard R. Clinical utility of cerebrospinal fluid biomarkers in the evaluation of cognitive impairment: a systematic review and meta-analysis. J Neurol Neurosurg Psychiatry 2023;94:113-120. 2022/09/13. DOI: 10.1136/jnnp-2022-329530.
134. ClinicalTrials.gov. Quality Improvement PrecivityAD Clinician Survey (QUIP I) https://clinicaltrials.gov/ct2/show/NCT05477056. Accessed Feb 2023.
© The Authors 2023